Connect With Us
Blog
Items filtered by date: February 2022
What Causes a Buildup of Uric Acid and Gout?
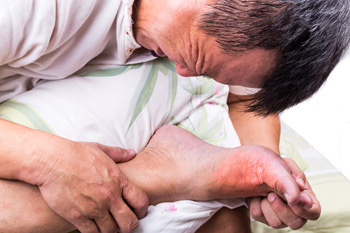 Gout, a type of arthritis that often affects the feet and toes, is caused by a buildup of uric acid in the bloodstream. About two-thirds of uric acid in the blood occurs naturally in the body, a product of the breakdown of cells. One-third of uric acid comes from eating foods that contain purines, chemicals that create uric acid as a byproduct when the body metabolizes them. When your body has high levels of uric acid, this substance can crystallize and lodge in your joints, causing painful gout flare-ups. Gout pain is typically sudden and severe, centered on an inflamed and swollen joint. If you have gout, it is suggested that you be under the care of a podiatrist.
Gout, a type of arthritis that often affects the feet and toes, is caused by a buildup of uric acid in the bloodstream. About two-thirds of uric acid in the blood occurs naturally in the body, a product of the breakdown of cells. One-third of uric acid comes from eating foods that contain purines, chemicals that create uric acid as a byproduct when the body metabolizes them. When your body has high levels of uric acid, this substance can crystallize and lodge in your joints, causing painful gout flare-ups. Gout pain is typically sudden and severe, centered on an inflamed and swollen joint. If you have gout, it is suggested that you be under the care of a podiatrist.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Dr. Richard Silverstein from Union Foot Care. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What Causes a Buildup of Uric Acid and Gout?
 Gout, a type of arthritis that often affects the feet and toes, is caused by a buildup of uric acid in the bloodstream. About two-thirds of uric acid in the blood occurs naturally in the body, a product of the breakdown of cells. One-third of uric acid comes from eating foods that contain purines, chemicals that create uric acid as a byproduct when the body metabolizes them. When your body has high levels of uric acid, this substance can crystallize and lodge in your joints, causing painful gout flare-ups. Gout pain is typically sudden and severe, centered on an inflamed and swollen joint. If you have gout, it is suggested that you be under the care of a podiatrist.
Gout, a type of arthritis that often affects the feet and toes, is caused by a buildup of uric acid in the bloodstream. About two-thirds of uric acid in the blood occurs naturally in the body, a product of the breakdown of cells. One-third of uric acid comes from eating foods that contain purines, chemicals that create uric acid as a byproduct when the body metabolizes them. When your body has high levels of uric acid, this substance can crystallize and lodge in your joints, causing painful gout flare-ups. Gout pain is typically sudden and severe, centered on an inflamed and swollen joint. If you have gout, it is suggested that you be under the care of a podiatrist.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Dr. Richard Silverstein from Union Foot Care. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about GoutIngrown Toenails 101
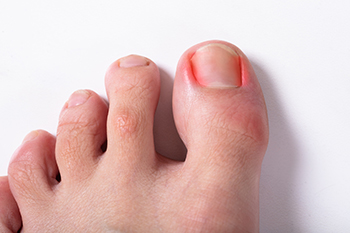 When the toenail becomes curved and grows into the skin along the sides of the nail, it forms an ingrown toenail. This can result in pain, inflammation, redness, swelling, and in some cases an infection. Issues such as genetics, improperly trimmed toenails, sweaty feet, and shoes that are too tight can all lead to ingrown toenails. In fact, athletes are particularly prone to ingrown toenails because they sweat more often. While ingrown toenails are usually not very serious, if left untreated, they can get very painful and may even get infected. Patients with ingrown toenails who have diabetes or a compromised immune system, have persistent pain, or believe that the nail is infected should consult with a podiatrist for treating the nail.
When the toenail becomes curved and grows into the skin along the sides of the nail, it forms an ingrown toenail. This can result in pain, inflammation, redness, swelling, and in some cases an infection. Issues such as genetics, improperly trimmed toenails, sweaty feet, and shoes that are too tight can all lead to ingrown toenails. In fact, athletes are particularly prone to ingrown toenails because they sweat more often. While ingrown toenails are usually not very serious, if left untreated, they can get very painful and may even get infected. Patients with ingrown toenails who have diabetes or a compromised immune system, have persistent pain, or believe that the nail is infected should consult with a podiatrist for treating the nail.
Ingrown toenails can become painful if they are not treated properly. For more information about ingrown toenails, contact Dr. Richard Silverstein of Union Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails occur when a toenail grows sideways into the bed of the nail, causing pain, swelling, and possibly infection.
Causes
- Bacterial infections
- Improper nail cutting such as cutting it too short or not straight across
- Trauma to the toe, such as stubbing, which causes the nail to grow back irregularly
- Ill-fitting shoes that bunch the toes too close together
- Genetic predisposition
Prevention
Because ingrown toenails are not something found outside of shoe-wearing cultures, going barefoot as often as possible will decrease the likeliness of developing ingrown toenails. Wearing proper fitting shoes and using proper cutting techniques will also help decrease your risk of developing ingrown toenails.
Treatment
Ingrown toenails are a very treatable foot condition. In minor cases, soaking the affected area in salt or antibacterial soaps will not only help with the ingrown nail itself, but also help prevent any infections from occurring. In more severe cases, surgery is an option. In either case, speaking to your podiatrist about this condition will help you get a better understanding of specific treatment options that are right for you.
If you have any questions please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Ingrown Toenails 101
 When the toenail becomes curved and grows into the skin along the sides of the nail, it forms an ingrown toenail. This can result in pain, inflammation, redness, swelling, and in some cases an infection. Issues such as genetics, improperly trimmed toenails, sweaty feet, and shoes that are too tight can all lead to ingrown toenails. In fact, athletes are particularly prone to ingrown toenails because they sweat more often. While ingrown toenails are usually not very serious, if left untreated, they can get very painful and may even get infected. Patients with ingrown toenails who have diabetes or a compromised immune system, have persistent pain, or believe that the nail is infected should consult with a podiatrist for treating the nail.
When the toenail becomes curved and grows into the skin along the sides of the nail, it forms an ingrown toenail. This can result in pain, inflammation, redness, swelling, and in some cases an infection. Issues such as genetics, improperly trimmed toenails, sweaty feet, and shoes that are too tight can all lead to ingrown toenails. In fact, athletes are particularly prone to ingrown toenails because they sweat more often. While ingrown toenails are usually not very serious, if left untreated, they can get very painful and may even get infected. Patients with ingrown toenails who have diabetes or a compromised immune system, have persistent pain, or believe that the nail is infected should consult with a podiatrist for treating the nail.
Ingrown toenails can become painful if they are not treated properly. For more information about ingrown toenails, contact Dr. Richard Silverstein of Union Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails occur when a toenail grows sideways into the bed of the nail, causing pain, swelling, and possibly infection.
Causes
- Bacterial infections
- Improper nail cutting such as cutting it too short or not straight across
- Trauma to the toe, such as stubbing, which causes the nail to grow back irregularly
- Ill-fitting shoes that bunch the toes too close together
- Genetic predisposition
Prevention
Because ingrown toenails are not something found outside of shoe-wearing cultures, going barefoot as often as possible will decrease the likeliness of developing ingrown toenails. Wearing proper fitting shoes and using proper cutting techniques will also help decrease your risk of developing ingrown toenails.
Treatment
Ingrown toenails are a very treatable foot condition. In minor cases, soaking the affected area in salt or antibacterial soaps will not only help with the ingrown nail itself, but also help prevent any infections from occurring. In more severe cases, surgery is an option. In either case, speaking to your podiatrist about this condition will help you get a better understanding of specific treatment options that are right for you.
If you have any questions please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Read more about Ingrown ToenailsReminder: When Was the Last Time...?
Reminder: When Was the Last Time...?
Potential Achilles Tendon Injuries
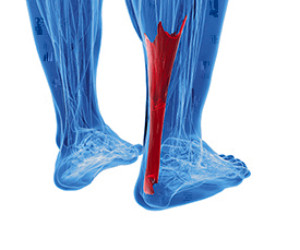 If you feel the back of your ankle, you will notice the fibrous tissue that connects the heel bone to the calf muscle. This is known as the Achilles tendon. There are two injuries that commonly affect this tendon. The first, known as Achilles tendinopathy, occurs when there is pain on the back of the heel as a result of overuse. Common signs of Achilles tendinopathy include swelling, stiffness, and pain that is worse in the morning. The second injury is an Achilles tendon rupture or tear, which commonly occurs as a result of jumping and pivoting with a lot of force. This causes the tendon to overstretch and eventually tear. Anyone who tears their Achilles tendon will notice a severe pain and a loss of both movement and strength in the tendon. If you are experiencing pain or swelling in your Achilles tendon, it is suggested that you consult with a podiatrist who can help provide a treatment option for injuries as well as ways to prevent a rupture.
If you feel the back of your ankle, you will notice the fibrous tissue that connects the heel bone to the calf muscle. This is known as the Achilles tendon. There are two injuries that commonly affect this tendon. The first, known as Achilles tendinopathy, occurs when there is pain on the back of the heel as a result of overuse. Common signs of Achilles tendinopathy include swelling, stiffness, and pain that is worse in the morning. The second injury is an Achilles tendon rupture or tear, which commonly occurs as a result of jumping and pivoting with a lot of force. This causes the tendon to overstretch and eventually tear. Anyone who tears their Achilles tendon will notice a severe pain and a loss of both movement and strength in the tendon. If you are experiencing pain or swelling in your Achilles tendon, it is suggested that you consult with a podiatrist who can help provide a treatment option for injuries as well as ways to prevent a rupture.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Dr. Richard Silverstein of Union Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Potential Achilles Tendon Injuries
 If you feel the back of your ankle, you will notice the fibrous tissue that connects the heel bone to the calf muscle. This is known as the Achilles tendon. There are two injuries that commonly affect this tendon. The first, known as Achilles tendinopathy, occurs when there is pain on the back of the heel as a result of overuse. Common signs of Achilles tendinopathy include swelling, stiffness, and pain that is worse in the morning. The second injury is an Achilles tendon rupture or tear, which commonly occurs as a result of jumping and pivoting with a lot of force. This causes the tendon to overstretch and eventually tear. Anyone who tears their Achilles tendon will notice a severe pain and a loss of both movement and strength in the tendon. If you are experiencing pain or swelling in your Achilles tendon, it is suggested that you consult with a podiatrist who can help provide a treatment option for injuries as well as ways to prevent a rupture.
If you feel the back of your ankle, you will notice the fibrous tissue that connects the heel bone to the calf muscle. This is known as the Achilles tendon. There are two injuries that commonly affect this tendon. The first, known as Achilles tendinopathy, occurs when there is pain on the back of the heel as a result of overuse. Common signs of Achilles tendinopathy include swelling, stiffness, and pain that is worse in the morning. The second injury is an Achilles tendon rupture or tear, which commonly occurs as a result of jumping and pivoting with a lot of force. This causes the tendon to overstretch and eventually tear. Anyone who tears their Achilles tendon will notice a severe pain and a loss of both movement and strength in the tendon. If you are experiencing pain or swelling in your Achilles tendon, it is suggested that you consult with a podiatrist who can help provide a treatment option for injuries as well as ways to prevent a rupture.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Dr. Richard Silverstein of Union Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Read more about What are Achilles Tendon InjuriesThe 8 Principles of Foot Ulcer Prevention for Diabetics
The presence of diabetic peripheral neuropathy (nerve damage) and peripheral artery disease (poor circulation) in many diabetic patients creates a perfect storm of factors that can make wounds difficult to detect and take longer to heal. Chronic wounds that don’t heal (ulcers) are potentially very dangerous to both the overall health of the patient as well as their affected limb. There are eight steps every diabetic should take to help prevent such ulcers: 1) check your feet daily for cuts, growths or red spots, 2) wash and thoroughly dry your feet every day, 3) moisturize your feet, except between the toes, 4) trim your toenails straight across, but not too short, 5) avoid walking barefoot, and wear shoes that fit well, 6) protect your feet from extreme heat or cold, 7) elevate your feet as much as possible when sitting, and exercise your toes and ankles to aid circulation, and 8) have a podiatrist examine your feet at least once a year.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dr. Richard Silverstein from Union Foot Care. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
The 8 Principles of Foot Ulcer Prevention for Diabetics
The presence of diabetic peripheral neuropathy (nerve damage) and peripheral artery disease (poor circulation) in many diabetic patients creates a perfect storm of factors that can make wounds difficult to detect and take longer to heal. Chronic wounds that don’t heal (ulcers) are potentially very dangerous to both the overall health of the patient as well as their affected limb. There are eight steps every diabetic should take to help prevent such ulcers: 1) check your feet daily for cuts, growths or red spots, 2) wash and thoroughly dry your feet every day, 3) moisturize your feet, except between the toes, 4) trim your toenails straight across, but not too short, 5) avoid walking barefoot, and wear shoes that fit well, 6) protect your feet from extreme heat or cold, 7) elevate your feet as much as possible when sitting, and exercise your toes and ankles to aid circulation, and 8) have a podiatrist examine your feet at least once a year.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dr. Richard Silverstein from Union Foot Care. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Read more about Wound CareBlog Archives
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016
- October 2016
- September 2016
- August 2016
- July 2016
- June 2016
- May 2016