Connect With Us

Key Facts About Bunions
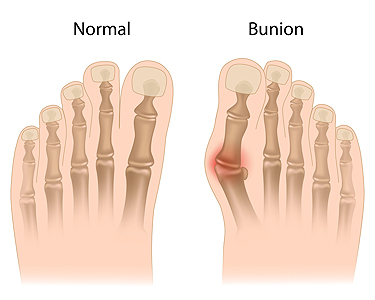
Bunions, a prevalent foot deformity, are characterized by a bony bump that forms at the base of the big toe. Contrary to common belief, bunions are not merely a cosmetic issue but can cause discomfort and affect mobility. One essential fact about bunions is their tendency to develop gradually over time, often due to structural issues in the foot, such as flat feet or abnormal bone alignment. Additionally, wearing ill-fitting shoes, particularly those with narrow toe boxes, can exacerbate bunion development or worsen existing symptoms. Individuals with bunions may experience pain, swelling, redness, and restricted movement in the affected toe. Despite popular misconceptions, bunions cannot be permanently corrected through nonsurgical means. However, conservative measures such as wearing supportive footwear, and using orthotic inserts can help alleviate symptoms and slow the progression of the deformity. For severe cases causing significant pain or hindering daily activities, surgical intervention may be necessary to realign the affected joint and provide lasting relief from bunions. If you have a bunion, it is suggested that you are under the care of a podiatrist who can help you to manage this condition.
If you are suffering from bunions, contact Dr. Richard Silverstein of Union Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions
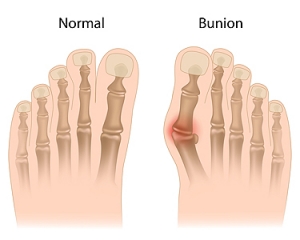
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.
Safeguarding Against Workplace Falls

Preventing falls in the workplace is essential in ensuring the safety and well-being of employees. Falls can occur in any work environment, from construction sites to office buildings, and can result in serious injuries or even fatalities. Implementing proactive measures to mitigate fall risks is vital. This includes maintaining clean and clutter-free walkways, promptly addressing spills or slippery surfaces, and ensuring proper lighting in all areas of the workplace. Employers should also provide appropriate training on fall prevention techniques and the proper use of safety equipment such as harnesses, guardrails, and non-slip footwear. Regular inspections of equipment and work areas can help identify and address potential hazards before accidents occur. Encouraging open communication between management and employees regarding safety concerns fosters a culture of awareness and accountability. Falling can impact the feet, and may compromise completing daily activities. If you have injured one or both feet during your workday, it is suggested that you consult a podiatrist who can treat any foot condition you may have endured.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Dr. Richard Silverstein from Union Foot Care. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Falls Prevention
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds, and every 19 minutes, an older person dies from falling. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
Proper Footwear for Medical Professionals

Selecting the appropriate footwear is important for medical employees, whose demanding roles require long hours of standing, walking, and patient care. The right shoes not only enhance comfort and alleviate fatigue but also play a critical role in preventing foot problems and injuries. Medical professionals often face unique challenges, such as exposure to bodily fluids, slippery surfaces, and the need for sterile environments. Therefore, shoes with non-slip soles, waterproof materials, and easy-to-clean surfaces are essential to ensure safety and hygiene. Additionally, supportive footwear with adequate cushioning, arch support, and shock absorption helps reduce strain on the feet, ankles, and lower back, minimizing the risk of musculoskeletal issues and promoting overall well-being. By investing in quality shoes that cater to their specific needs, medical employees can maintain optimal performance and focus on patient care. If you have foot pain from wearing shoes that do not fit well during your work day, it is suggested that you contact a podiatrist who can offer help to remedy your discomfort.
While working on the feet, it is important to take the proper care of them. For more information about working on your feet, contact Dr. Richard Silverstein from Union Foot Care. Our doctor will treat your foot and ankle needs.
Working on Your Feet
Standing on your feet for long periods of time can cause stress and pain in your feet. Your whole body may experience change in terms of posture, back pain, bunions, callouses and or plantar warts. There are ways to avoid these conditions with proper foot care, smart choices and correct posture.
Positive Changes
Negative heeled shoe – Choosing this shoe type places the heel slightly lower than the ball of the foot. These are great for overall foot health. Find shoes that fit you correctly.
Go barefoot – Our feet were not designed to be enclosed for all hours of the day. Try to periodically expose your feet to air.
Eliminate Pain
Foot Exercises – Performing simple exercises, incorporating yoga and doing stretches are beneficial. This will allow increased blood flow to the area and muscles of the foot.
Achilles tendon – Stretching the foot out flat on the floor will relax the calf muscles and tendon. These exercises can be performed almost anywhere. Make sure you add these exercises to your daily regimen.
With a little bit of this information and knowing more about foot health, you will notice changes. Foot stretches and proper footwear will help with pain and prevent further issues.
If you have any questions please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Working on Your Feet
Foot care is important regardless of your profession, but those who work on their feet must pay special attention. Bunions, calluses, blisters, and plantar warts are just a few of the many conditions that can arise after standing all day. While painful at their worst, these conditions can easily be avoided with the right foot care. This includes both appropriate footwear and proper posture—important elements that affect the health of your feet.
Choosing appropriate footwear means choosing a shoe that has a negative heel. This means that the heel is slightly lower than the ball of your foot, which places less of a strain. If you have a profession that requires you to be on your feet all day, investing in a pair of high-quality shoes is pertinent. High-quality shoes can be purchased from a respected manufacturer that emphasizes foot care and foot health.
Despite the regularity of wearing shoes, the feet are naturally not designed to be enclosed. Regular “barefoot” time for your feet can be beneficial for foot health. Among other methods, allowing your feet to breathe can help alleviate the pain and pressure your feet may be experiencing from being on your feet all day.
Simple foot exercises and yoga positions can help improve both the health and function of your feet. Active foot exercises that create movement will stimulate your foot’s blood flow and circulation, and yoga positions that place your feet flat onto the floor will stretch out their muscles. Yoga is particularly beneficial for your Achilles tendon and calf muscles, which are areas that can become especially problematic if not taken care of. Foot exercises and yoga positions can be easily performed every day at virtually any location and any time; whether it is at the office, at the gym, or at home right before you go to bed. Simple stretching can increase your foot health by miles.
The foot pain you experience after lengthy hours working on your feet may seem inevitable and unavoidable; in reality, however, that is not the case. Wearing proper footwear and performing simple foot exercises and stretches can help ease foot pain and allow you to truly avoid frustrating foot problems.
Your feet can easily be kept healthy with some education and a little effort. Pain that begins at the feet can eventually affect the whole body. Begin taking care of your feet now!
What is Plantar Fasciitis?
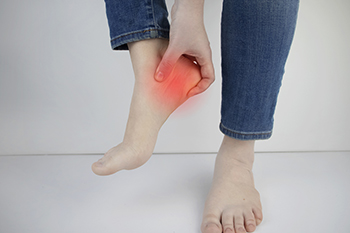
Plantar fasciitis is a prevalent foot condition characterized by inflammation of the plantar fascia, a thick band of tissue that runs across the bottom of the foot, connecting the heel bone to the toes. The primary cause of plantar fasciitis is the excessive or repetitive strain on the ligament, leading to tiny tears and inflammation. This strain can result from various factors, including prolonged standing or walking, wearing improper footwear, engaging in high-impact activities like running or jumping, and certain biomechanical issues such as flat feet or high arches. A common symptom of plantar fasciitis is heel pain, particularly when taking the first steps after waking up or after long periods of rest. This pain may gradually subside with movement but can worsen throughout the day with prolonged activity. Additionally, individuals with plantar fasciitis may experience stiffness and tenderness on the bottom of the foot, particularly near the heel. If you have heel pain, it is strongly suggested that you consult a podiatrist who can accurately diagnose and treat plantar fasciitis.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. Richard Silverstein from Union Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
Definition and Risk Factors of Sever’s Disease
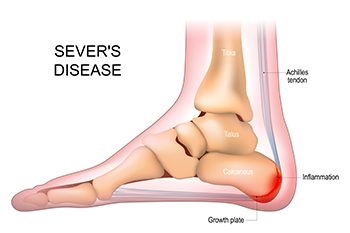
Sever's disease, also known as calcaneal apophysitis, is a common condition affecting children and adolescents, particularly those engaged in physical activities such as running or jumping. It occurs when the growth plate at the back of the heel bone becomes inflamed due to repetitive stress or tension. The growth plate, known as the calcaneal apophysis, is a vulnerable area where new bone forms as children grow. Common causes of Sever's disease include overuse, rapid growth spurts, and participation in high-impact sports that place excessive strain on the heel bone. Symptoms typically include heel pain, especially during physical activity or when pressing the affected area. Children may also experience swelling and tenderness at the back of the heel. Those participating in sports or activities involving repetitive pounding on hard surfaces are at higher risk of developing Sever's disease. If you notice your active child has heel pain or is limping, it is suggested that you consult a podiatrist who can diagnose and treat Sever’s disease and other foot problems.
Sever's disease often occurs in children and teens. If your child is experiencing foot or ankle pain, see Dr. Richard Silverstein from Union Foot Care. Our doctor can treat your child’s foot and ankle needs.
Sever’s Disease
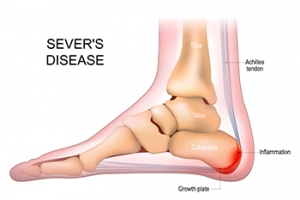
Sever’s disease is also known as calcaneal apophysitis, which is a medical condition that causes heel pain I none or both feet. The disease is known to affect children between the ages of 8 and 14.
Sever’s disease occurs when part of the child’s heel known as the growth plate (calcaneal epiphysis) is attached to the Achilles tendon. This area can suffer injury when the muscles and tendons of the growing foot do not keep pace with bone growth. Therefore, the constant pain which one experiences at the back of the heel will make the child unable to put any weight on the heel. The child is then forced to walk on their toes.
Symptoms
Acute pain – Pain associated with Sever’s disease is usually felt in the heel when the child engages in physical activity such as walking, jumping and or running.
Highly active – Children who are very active are among the most susceptible in experiencing Sever’s disease, because of the stress and tension placed on their feet.
If you have any questions, please feel free to contact our office located in Havre de Grace, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle injuries.